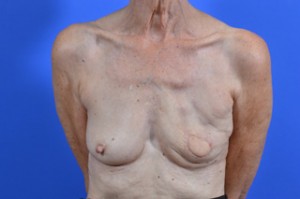
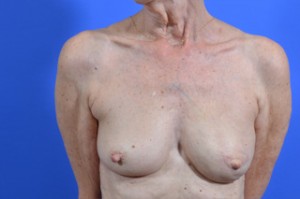
Latissimus Flap with Implant Breast Reconstruction (2-stage)
Conveniently located to serve St. Louis, Missouri
Jump To:
 The latissimus muscle flap is a versatile procedure that has been used for decades. The latissimus muscle is a muscle in the back that can be used for reconstruction without disabling a patient. The muscle may be used by itself or in conjunction with an implant to reconstruct a breast, depending on the situation. The muscle can be used to reconstruct an entire breast in the situation where a woman does not desire a prosthetic implant to be placed or to match a natural breast. The latissimus is also commonly used in situations where a breast has been radiated to reverse the radiation damage.
The latissimus muscle flap is a versatile procedure that has been used for decades. The latissimus muscle is a muscle in the back that can be used for reconstruction without disabling a patient. The muscle may be used by itself or in conjunction with an implant to reconstruct a breast, depending on the situation. The muscle can be used to reconstruct an entire breast in the situation where a woman does not desire a prosthetic implant to be placed or to match a natural breast. The latissimus is also commonly used in situations where a breast has been radiated to reverse the radiation damage.
If a woman desires or requires more volume than the latissimus flap can provide, an implant may be used. In the setting of previous radiation to the breast, the latissimus flap can help reverse the radiation damage and can improve the overall contour and shape of the reconstruction. An example would be a patient that has a previous reconstruction and has a high implant, a condition known as capsular contracture. The flap can be used to correct this.
Candidates
Candidates for this procedure include patients who have already had a mastectomy and radiation. Due to the radiation damage to the chest muscle, the muscle will not easily stretch and does not accommodate an implant of any sort. Also, women who had a previous tissue expander reconstruction which failed may be candidates.
Preparing for Surgery
Dr. Cabbabe will ask that you refrain from taking any aspirin, plavix, Coumadin, ibuprofen or any other type of blood thinner. If you are taking chemotherapy, this will need to be finished prior to surgery.
Before & After Gallery
View before-and-after pictures of real patients of Cabbabe Plastic Surgery
Surgery
In this procedure, the entire latissimus muscle along with a strip of skin attached is pivoted and transferred from the back into the breast under the skin. A temporary tissue expander is placed between the latissimus muscle and the chest muscle. A horizontal scar from the back where the muscle was removed will be able to be concealed by a bra. The skin from the back replaces missing skin on the breast from the mastectomy and also gets stretched during the expansion process.
If a skin sparing mastectomy is being done, an implant can be placed underneath the muscle at the time of mastectomy for a one – stage reconstruction (latissimus with implant). You would not want to do this if radiation is to be done after the procedure as this would damage the latissimus muscle.
The tissue expander is inflated in the office regularly after surgery to the desired size. A second stage operation is done after this size has been achieved to replace the tissue expander with a permanent saline or silicone implant. Additional fat grafting is done as needed to contour the breast. The pocket around the expander is modified at the time of surgery to optimize the aesthetic result.
A breast lift or breast reduction may be needed on the other breast in order to improve symmetry. A new nipple can be made and areolar tattooing can be done if desired in the case of mastectomy.
Your Latissimus Flap with Implant Breast Reconstruction (2-stage) will be performed in a hospital or surgery center in St. Louis, MO.
Recovery
Patients are admitted to the hospital overnight. Pain medication and antibiotics will be prescribed. There may be some numbness on the breast and back which improve with time. Most patients are able to shower within 24 hours. A drain will be placed inside the breast and one or two in the back and removed in the office. These will stay in place for 1-3 weeks. Recovery is 3 to 4 weeks approximately.
Complications
The most common complication is a fluid collection which can form in the back where the muscle was removed after the drains have been removed. This occurs in up to 33% of patients and require a simple aspiration of the fluid with a syringe and needle in the office. The blood vessels to the muscle flap can be injured as a result of the procedure or the previous lymph node surgery and the muscle flap could lose blood flow, turn black and require further surgery to remove. Patients can have some shoulder weakness for the first few months but this gradually improves.
Types of Reconstruction:
- Fat Grafting
- Oncoplastic Breast Reconstruction (one – stage)
- Tissue Expander – Implant (two – stage)
- Tissue Expander – Implant with Acellular Dermis (two –stage)
- Implant with Acellular Dermis (one-stage)
- Latissimus Flap (one – stage)
- Latissimus Flap with Expander – Implant (two – stage)
- Latissimus Flap with Implant (one-stage)
- Conventional TRAM (one – stage)
- Free Muscle – Sparing TRAM (one –stage)
- DIEP Flap (one – stage)
- SIEA Flap (one – stage)
- SGAP/LGAP (one – stage)
- Fat Transfer Breast Augmentation
- Breast Implant Reconstruction (One-stage)
- Breast Implant Revision Surgery
- Breast Tissue Expander – Implant Reconstruction (2-stage)
- Latissimus Flap Breast Reconstruction
- Latissimus Flap Breast Reconstruction with Implant (1-stage)
- Latissimus Flap with Implant Breast Reconstruction (2-stage)
- Transverse Upper Gracilis (TUG) Flap Breast Reconstruction