DIEP Flap
Conveniently located to serve St. Louis, Missouri
Jump To:
 A TRAM (Transverse Rectus Abdominis Myocutaneous) flap is a procedure where skin and fat from the lower abdomen is used to reconstruct the entire breast. In this situation, no implants are used and either one or both breasts can be reconstructed. Women who have had this procedure describe the breast as “their own” as opposed to an implant – based reconstruction. Compared to a conventional TRAM where the entire rectus (six-pack) muscle is removed along with the flap, the MS-TRAM (muscle – sparing TRAM) involves removal of a small portion of the muscle followed by microsurgical (surgery under a microscope to connect blood vessels) reconstruction . This spares the abdominal muscles, leads to quicker recovery and long – term strength of the abdomen. A deep inferior epigastric artery perforator (DIEP) flap, on the other hand, involves no removal of abdominal muscle. Instead, the blood vessels (artery and vein) to the tissue are removed from within the muscle without removing any actual muscle. This leads to quicker recovery and less abdominal weakness or complications long – term.
A TRAM (Transverse Rectus Abdominis Myocutaneous) flap is a procedure where skin and fat from the lower abdomen is used to reconstruct the entire breast. In this situation, no implants are used and either one or both breasts can be reconstructed. Women who have had this procedure describe the breast as “their own” as opposed to an implant – based reconstruction. Compared to a conventional TRAM where the entire rectus (six-pack) muscle is removed along with the flap, the MS-TRAM (muscle – sparing TRAM) involves removal of a small portion of the muscle followed by microsurgical (surgery under a microscope to connect blood vessels) reconstruction . This spares the abdominal muscles, leads to quicker recovery and long – term strength of the abdomen. A deep inferior epigastric artery perforator (DIEP) flap, on the other hand, involves no removal of abdominal muscle. Instead, the blood vessels (artery and vein) to the tissue are removed from within the muscle without removing any actual muscle. This leads to quicker recovery and less abdominal weakness or complications long – term.
Candidates
Candidates for this procedure include patients who are having or have had a mastectomy or are unhappy with a previous expander/implant reconstruction. Patients with previous radiation are also excellent candidates for this procedure. If radiation is anticipated, then the procedure will be delayed until after radiation is completed so as not to permanently damage the abdominal tissue from the radiation. In this situation, a temporary implant, or expander, may be used to preserve as much skin as possible on the breast until the final reconstruction is done.
Poor candidates for this surgery are women who are significantly obese (BMI >35) as this may lead to problems with abdominal hernias and/or poor blood flow to the abdominal tissue which can result in failure. Also, patients with previous abdominal surgeries may not be candidates depending on the location of their scars. Patients who smoke have a greater risk of complications due to poor blood flow and coughing. Finally, women who have little fat on their lower abdomen may not be able to attain the breast size they desire. Fat transfer to the flap can be done in some instances to increase the volume of the flap in a later surgery revision.
Preparing for Surgery
Dr. Cabbabe will ask that you refrain from taking any aspirin, plavix, Coumadin, ibuprofen or any other type of blood thinner. If you are taking chemotherapy, this will need to be finished prior to surgery.
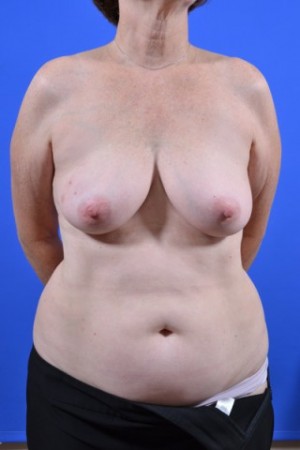
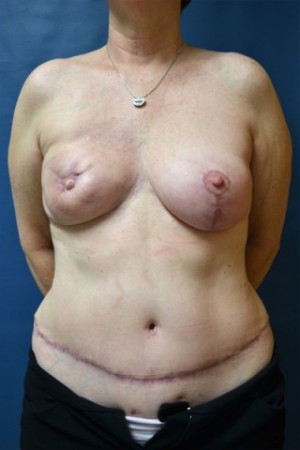
Before & After Gallery
View before-and-after pictures of real patients of Cabbabe Plastic Surgery
Surgery
During the procedure the abdominal tissue from the lower abdomen is transferred with an artery and vein to the “flap” up into the breast. The blood vessels are removed from within the abdominal muscles. Blood vessels between the ribs are identified to provide inflow of blood into and out of the skin and fat from the abdomen. Under a microscope, the artery and vein (s) are reconnected with fine sutures to re-establish blood flow to the flap. The breast is then shaped and molded on the chest to recreate the breast. If you are having a double or bilateral mastectomy, the same procedure is repeated on both sides.
The area on the abdomen from which the muscle was taken is closed, occasionally with mesh reinforcement, and the belly button/umbilicus is preserved and transposed to a new position after the remaining skin of the abdomen is stretched down. This is much like a tummy tuck with the exception of removal of a small portion of the muscles.
A breast lift or reduction may be needed on the other breast in order to improve symmetry if one breast only is removed. A new nipple can be made and areolar tattooing can be done if desired in the case of skin sparing mastectomy. This procedure can only be done once in a person’s lifetime in case a patient is considering a unilateral reconstruction then later have a mastectomy on the other side.
Your DIEP Flap will be performed in a hospital or surgery center in St. Louis, MO.
Recovery
You will be admitted to the hospital for two to four nights. Pain medication and antibiotics will be prescribed. An epidural may be used depending on the situation. There may be some numbness on the breast and abdomen which gradually improve with time. Most patients are able to shower within 24-48 hours. Drains will be placed inside the breast and in the abdomen for approximately 2 weeks. Recovery is approximately 4 to 6 weeks. There may be some residual weakness of the abdominal wall after surgery. Most patients are kept on aspirin for 6 weeks after surgery to prevent clotting of the vessel anastomosis/connection.
Complications
A fluid collection can form in the abdomen where the tissue was removed after the drains have been removed. This occurs in up to 20% of patients and require a simple aspiration of the fluid with a syringe and needle in the office. The blood vessels to the tissue flap can be injured as a result of the procedure or the blood vessel connection can clot after surgery, requiring an emergent return to the operating room to salvage the reconstruction. The flap could lose blood flow, turn black and require further surgery to remove. Patients can have some abdominal weakness for the first few months but this gradually improves. Bulging of the abdomen may occur after surgery due to weakness and require further surgery.
Types of Reconstruction:
- Fat Grafting
- Oncoplastic Breast Reconstruction (one – stage)
- Tissue Expander – Implant (two – stage)
- Tissue Expander – Implant with Acellular Dermis (two –stage)
- Implant with Acellular Dermis (one-stage)
- Latissimus Flap (one – stage)
- Latissimus Flap with Expander – Implant (two – stage)
- Latissimus Flap with Implant (one-stage)
- Conventional TRAM (one – stage)
- Free Muscle – Sparing TRAM (one –stage)
- DIEP Flap (one – stage)
- SIEA Flap (one – stage)
- SGAP/LGAP (one – stage)
- Fat Transfer Breast Augmentation
- Breast Implant Reconstruction (One-stage)
- Breast Implant Revision Surgery
- Breast Tissue Expander – Implant Reconstruction (2-stage)
- Latissimus Flap Breast Reconstruction
- Latissimus Flap Breast Reconstruction with Implant (1-stage)
- Latissimus Flap with Implant Breast Reconstruction (2-stage)
- Transverse Upper Gracilis (TUG) Flap Breast Reconstruction