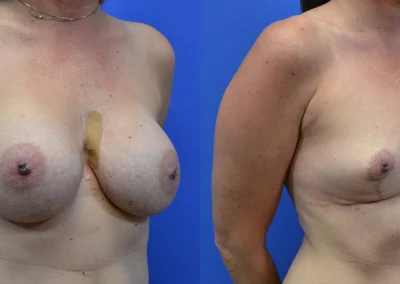
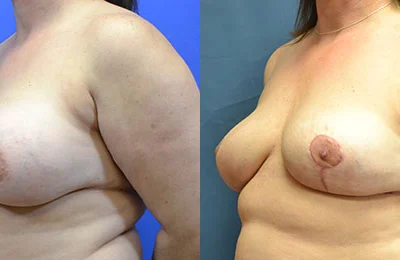
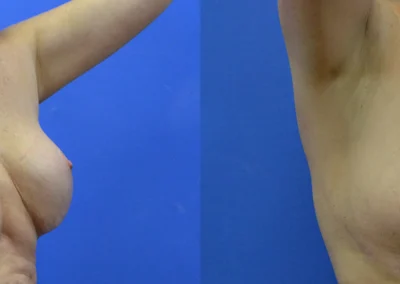
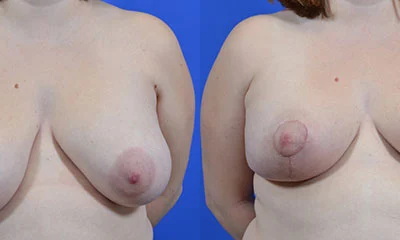
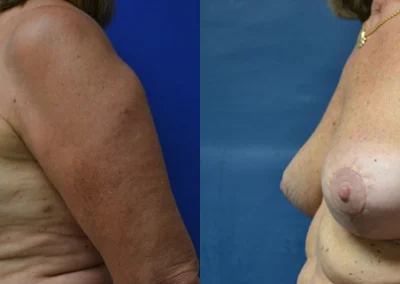
Breast Implant Removal
Breast Implant Removal (Explant Surgery): En Bloc vs Total Capsulectomy vs Partial Capsulectomy
Why Do Women Seek Breast Implant Removal?
Women seek breast implant removal for many reasons, including:
- Capsular contracture
- Implant malposition
- Implant rupture
- Bottoming out or sinking implants
- Pain or discomfort
- Implants that feel too large or heavy
- Dissatisfaction with appearance
- Concerns about Breast Implant Illness (BII)
It is important to understand that the surgical plan should be tailored to the specific diagnosis and the patient’s goals. Explant surgery is not a one-size-fits-all operation.
In some patients, a revision augmentation — such as downsizing implants, changing implant position, correcting capsular contracture, or adding internal support such as mesh — may actually improve symptoms like pain, heaviness, and implant malposition better than explant alone. The correct operation depends on the underlying problem, so it is important for patients to come to consultation with an open mind.
What Is the Capsule Around a Breast Implant?
The capsule around a breast implant is scar tissue. It is not an implant, a toxin, or a foreign device — it is the body’s normal scar response, similar to scar tissue that forms after any surgery.
In most areas of the body, we do not routinely remove all scar tissue because doing so can increase surgical risk and create unnecessary trauma. The same principle applies in breast surgery.
En Bloc vs Total Capsulectomy vs Partial Capsulectomy
This is one of the most misunderstood topics in breast surgery.
- En bloc capsulectomy: Implant and capsule removed together in one piece. This is primarily a cancer operation, most commonly performed in cases such as BIA-ALCL.
- Total capsulectomy: All capsule is removed, but not necessarily in one piece.
- Partial capsulectomy: Only part of the capsule is removed and the remaining capsule is treated or the pocket is closed.
These are three different operations with different indications, risks, and goals. Many patients use the term en bloc when they are actually referring to a total capsulectomy.
Does Total Capsulectomy Help Breast Implant Illness (BII)?
Current studies have not shown a clear or consistent benefit that total capsulectomy improves symptoms of Breast Implant Illness (BII) compared to other forms of implant removal.
However, what we do know is that total capsulectomy is a more aggressive operation and carries higher surgical risk, including:
- Longer surgery
- Increased pain after surgery
- Higher risk of bleeding
- Higher complication rates
- Increased risk of contour irregularities visible through the breast after implant removal
More aggressive surgery is not always better surgery.
Implant Location Matters: Above vs Below the Muscle
The ability to perform a total capsulectomy depends heavily on implant location.
- Above the muscle: Capsule is often easier and safer to remove.
- Below the muscle: Capsule is often stuck to the ribs and chest wall and can be very difficult — and sometimes unsafe — to remove completely.
If a surgeon guarantees an en bloc or total capsulectomy for implants below the muscle in every case, that is often not realistic and may not accurately reflect the surgical risks and anatomical limitations.
Why Closing the Pocket Is Often More Important Than Removing All Capsule
During explant surgery, one of the most important steps is properly closing and managing the implant pocket.
In many cases, safely removing the implant and closing the pocket so the body can heal and scar that space down is more important than aggressively trying to remove every millimeter of capsule, which can increase risk without proven additional benefit.
Risks of Aggressive Capsule Removal
Patients need to understand that aggressive capsule removal can:
- Increase pain after surgery
- Increase bleeding risk
- Increase complication risk
- Increase the risk of contour irregularities
- Remove tissue that may actually be helping support breast shape
More aggressive surgery is not always better — and in some cases may lead to worse cosmetic outcomes.
Do You Need a Breast Lift at the Time of Explant?
We cannot guarantee breast shape after implant removal, and a breast lift is not always beneficial at the time of explant.
In women with small breasts and minimal sagging, a breast lift is essentially a breast reduction — it adds scars and often makes the breast smaller without significantly improving shape. In these patients, a lift may not be worthwhile.
In some cases, fat transfer can be considered to help improve contour after explant, but patients must understand that fat transfer requires liposuction to obtain fat and is therefore a more involved body contouring procedure.
Patients should not be misled into thinking that an en bloc capsulectomy and a breast lift will fix everything. These decisions should be made carefully based on anatomy and goals.
Key Takeaways – Breast Implant Removal
- The capsule is scar tissue, not a toxin or implant.
- En bloc, total, and partial capsulectomy are different surgeries.
- En bloc capsulectomy is primarily a cancer operation.
- Total capsulectomy has higher risks, including bleeding and pain.
- Implants under the muscle are often not safely removable en bloc.
- Closing the implant pocket is often more important than removing all capsule.
- A breast lift is not always beneficial at the time of explant.
- Fat transfer may be an option in some patients.
- The goal is not the most aggressive surgery — it is the safest and most appropriate surgery.
Final Thoughts
Breast implant removal, en bloc capsulectomy, total capsulectomy, and partial capsulectomy are different operations with different indications and different risk profiles. This is not a one-size-fits-all situation.
The goal is not to perform the most aggressive operation — the goal is to perform the right operation for the diagnosis, in the safest way possible.
The Surgery
Incisions are made based on pre-operative markings and planning. An incision under the breast is preferred due to the size needed for implant and capsule removal. A lift may be incorporated as needed depending on the droopiness of the breast or the location of the nipple – areola.
Antibiotics are given before the procedure and early range of motion is done with the arms. Patients will generally follow-up within 1 day to 1 week and then approximately 3-4 weeks later and then in several months. Drains are removed 1-2 weeks after surgery depending on the extent of the procedure.
Nipple sensation and the ability to lactate are usually preserved in these procedures but there is a risk of loss of nipple sensation.
Preparing for Surgery
Dr. Cabbabe will ask that you refrain from taking any aspirin, plavix, Coumadin, ibuprofen or any other type of blood thinner. If you are older than 40, a mammogram within one year prior to the procedure is recommended as part of normal health screening.
Recovery
Recovery is approximately 1-2 weeks depending on the extent of the procedure and the type of work one does. Most women who have this procedure done will be up and about the next day, moving around although they may need pain medication occasionally, but most women state it was not as bad as they anticipated and most of them, if they’ve had it done on a Thursday or Friday, can usually return to work within 1 week.
Dr. Cabbabe strives to make the procedure as easy and comfortable as possible for his patients. Before surgery, patients usually receive anti-inflammatory pain medications that do not cause bleeding. At the time of surgery, local anesthesia numbing medicine is used that is long – lasting into the breast. After surgery, early range of motion is begun and pain medications are given.
Risks
The complications that can occur include infections, fluid collections after drain removal and bleeding requiring further surgery to evacuate blood or stop bleeding. Most women have some asymmetry to their breasts and this may be present after surgery unless a recommendation is made to perform a lift or reduction.